
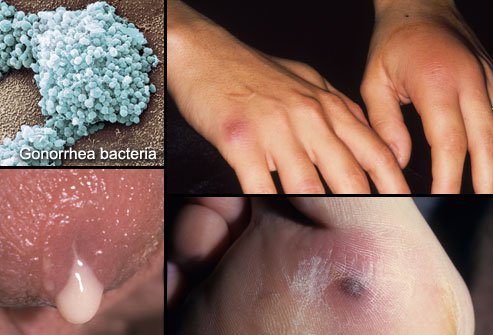
Female reproductive systemThe ovaries, fallopian tubes, uterus, cervix and vagina (vaginal canal) make up the female reproductive system.In many cases, gonorrhea infection causes no symptoms. Symptoms, however, can affect many sites in your body, but commonly appear in the genital tract. Gonorrhea affecting the genital tractSigns and symptoms of gonorrhea infection in men include:. Painful urination.
Gonorrhea is a sexually transmitted disease (STD). You get it from having sex with someone who is infected with it. You may have heard people call it “the clap. Chlamydia is more common than gonorrhea. According to a 2017 report, over 1.7 million cases of chlamydia were reported in the United States, while just over 550,000 cases of gonorrhea were documented.
Pus-like discharge from the tip of the penis. Pain or swelling in one testicleSigns and symptoms of gonorrhea infection in women include:. Increased vaginal discharge. Painful urination. Vaginal bleeding between periods, such as after vaginal intercourse. Abdominal or pelvic painGonorrhea at other sites in the bodyGonorrhea can also affect these parts of the body:. Rectum.
Signs and symptoms include anal itching, pus-like discharge from the rectum, spots of bright red blood on toilet tissue and having to strain during bowel movements. Eyes. Gonorrhea that affects your eyes can cause eye pain, sensitivity to light, and pus-like discharge from one or both eyes. Throat.
Signs and symptoms of a throat infection might include a sore throat and swollen lymph nodes in the neck. Joints. If one or more joints become infected by bacteria (septic arthritis), the affected joints might be warm, red, swollen and extremely painful, especially during movement.When to see your doctorMake an appointment with your doctor if you notice any troubling signs or symptoms, such as a burning sensation when you urinate or a pus-like discharge from your penis, vagina or rectum.Also make an appointment with your doctor if your partner has been diagnosed with gonorrhea. You may not experience signs or symptoms that prompt you to seek medical attention. But without treatment, you can reinfect your partner even after he or she has been treated for gonorrhea.
CausesGonorrhea is caused by the bacterium Neisseria gonorrhoeae. The gonorrhea bacteria are most often passed from one person to another during sexual contact, including oral, anal or vaginal intercourse. Risk factorsSexually active women younger than 25 and men who have sex with men are at increased risk of getting gonorrhea.Other factors that can increase your risk include:. Having a new sex partner.
Having a sex partner who has other partners. Having more than one sex partner. Having had gonorrhea or another sexually transmitted infectionComplicationsUntreated gonorrhea can lead to major complications, such as:.
Infertility in women. Gonorrhea can spread into the uterus and fallopian tubes, causing pelvic inflammatory disease (PID). PID can result in scarring of the tubes, greater risk of pregnancy complications and infertility. PID requires immediate treatment. Infertility in men. Gonorrhea can cause a small, coiled tube in the rear portion of the testicles where the sperm ducts are located (epididymis) to become inflamed (epididymitis). Untreated epididymitis can lead to infertility.
Infection that spreads to the joints and other areas of your body. The bacterium that causes gonorrhea can spread through the bloodstream and infect other parts of your body, including your joints.
Fever, rash, skin sores, joint pain, swelling and stiffness are possible results. Increased risk of HIV/AIDS. Having gonorrhea makes you more susceptible to infection with human immunodeficiency virus (HIV), the virus that leads to AIDS. People who have both gonorrhea and HIV are able to pass both diseases more readily to their partners. Complications in babies.
Babies who contract gonorrhea from their mothers during birth can develop blindness, sores on the scalp and infections.PreventionTo reduce your gonorrhea risk:. Use a condom if you have sex. Abstaining from sex is the surest way to prevent gonorrhea. But if you choose to have sex, use a condom during any type of sexual contact, including anal sex, oral sex or vaginal sex. Limit your number of sex partners. Being in a monogamous relationship in which neither partner has sex with anyone else can lower your risk. Be sure you and your partner are tested for sexually transmitted infections.
Before you have sex, get tested and share your results with each other. Don't have sex with someone who appears to have a sexually transmitted infection. If your partner has signs or symptoms of a sexually transmitted infection, such as burning during urination or a genital rash or sore, don't have sex with that person.Consider regular gonorrhea screening. Annual screening is recommended for sexually active women younger than 25 and for older women at increased risk of infection.
This includes women who have a new sex partner, more than one sex partner, a sex partner with other partners, or a sex partner who has a sexually transmitted infection.Regular screening is also recommended for men who have sex with men, as well as their partners.To avoid getting gonorrhea again, abstain from sex until after you and your sex partner have completed treatment and after symptoms are gone. Gonorrhea: CDC fact sheet (detailed version). Centers for Disease Control and Prevention. Accessed Sept. 14, 2019.
Ghanem KG. Clinical manifestations and diagnosis of Neisseria gonorrhoeae infection in adults and adolescents. Accessed Sept.
14, 2019. Gonorrhea. Office on Women's Health.
Accessed Sept. 14, 2019. Gonorrhea. Merck Manual Professional Version. Accessed Sept. 14, 2019.
AskMayoExpert. Chlamydia, gonorrhea, and nongonococcal urethritis. Mayo Clinic; 2019. Speer ME.
Gonococcal infection in the newborn. Accessed Sept.
. /ˌɡɒn.əˈɹi.ə/SymptomsNone, discharge from the,CausestypicallyTesting the urine, in males, or in femalesPrevention, having sex with only one person who is uninfected,Treatmentby injection and by mouthFrequency0.8% (women), 0.6% (men)Gonorrhea, colloquially known as the clap, is a (STI) caused by the bacterium. Infection may involve the, mouth, and/or. Infected men may experience, discharge from the,.
Infected women may experience burning with urination, vaginal bleeding between,. Complications in women include and in men include.
Many of those infected, however, have no symptoms. If untreated, gonorrhea can spread to or.Gonorrhea is spread through sexual contact with an infected person. This includes oral, anal, and vaginal sex. It can also spread from a. Diagnosis is by testing the urine, in males, or in females. Testing all women who are sexually active and less than 25 years of age each year as well as those with new sexual partners is recommended; the same recommendation applies in (MSM).Gonorrhea can be prevented with the use of, having sex with only one person who is uninfected,. Treatment is usually with by injection and by mouth.
Has developed to many previously used and higher doses of ceftriaxone are occasionally required. Retesting is recommended three months after treatment. Sexual partners from the last two months should also be treated.Gonorrhea affects about 0.8% of women and 0.6% of men. An estimated 33 to 106 million new cases occur each year, out of the 498 million new cases of curable STI – which also includes,. Infections in women most commonly occur when they are young adults. In 2015, it caused about 700 deaths. Descriptions of the disease date back to before the within the.
The current name was first used by the Greek physician before 200 CE who referred to it as 'an unwanted discharge of semen'. Contents.Signs and symptomsGonorrhea infections of can cause swelling, itching, pain, and the formation of.
The is usually between two and 14 days, with most symptoms appearing between four and six days after infection, if they appear at all. Both men and women with infections of the throat may experience a, though such infection does not produce symptoms in 90% of cases. Other symptoms may include swollen lymph nodes around the neck.
Either sex can become infected in the eyes or rectum if these tissues are exposed to the bacterium.WomenHalf of women with gonorrhea are but the other half experience, lower abdominal pain, or associated with. Common medical complications of untreated gonorrhea in women include which can cause scars to the and result in later among those women who become pregnant. MenMost infected men with symptoms have associated with a and discharge from the penis. In men, discharge with or without burning occurs in half of all cases and is the most common symptom of the infection. This pain is caused by a narrowing and stiffening of the urethral. The most common medical complication of gonorrhea in men is.
Gonorrhea is also associated with increased risk of. An infant with gonorrhea of the eyesIf not treated, will develop in 28% of infants born to women with gonorrhea. SpreadIf left untreated, gonorrhea can spread from the original site of infection and infect and damage the joints, skin, and other organs. Indications of this can include fever, skin rashes, sores, and joint pain and swelling. In advanced cases, gonorrhea may cause a general similar to other infections.
It is also possible for an individual to have an to the bacteria, in which case any appearing symptoms will be greatly intensified. Very rarely it may settle in the heart causing or in the spinal column causing (both are more likely among individuals with suppressed immune systems, however). Multiple views of a bacterium, which causes gonorrhea.Gonorrhea is caused by the bacterium. Previous infection does not confer immunity – a person who has been infected can become infected again by exposure to someone who is infected.
Infected persons may be able to infect others repeatedly without having any signs or symptoms of their own.SpreadThe infection is usually spread from one person to another through,. Men have a 20% risk of getting the infection from a single act of vaginal intercourse with an infected woman. The risk for men that have sex with men (MSM) is higher.
Active MSM may get a penile infection, while passive MSM may get anorectal gonorrhea. Women have a 60–80% risk of getting the infection from a single act of vaginal intercourse with an infected man.A mother may transmit gonorrhea to her newborn during childbirth; when affecting the infant's eyes, it is referred to as.
It may be able to spread through the objects contaminated with body fluid from an infected person. The bacteria typically does not survive long outside the body, typically dying within minutes to hours. DiagnosisTraditionally, gonorrhea was diagnosed with and; however, newer (PCR)-based testing methods are becoming more common. In those failing initial treatment, culture should be done to determine sensitivity to antibiotics.Tests that use (, aka nucleic acid amplification) to identify genes unique to N. Gonorrhoeae are recommended for screening and diagnosis of gonorrhea infection.
These PCR-based tests require a sample of urine, urethral swabs, or cervical/vaginal swabs. Culture (growing colonies of bacteria in order to isolate and identify them) and Gram-stain (staining of bacterial cell walls to reveal morphology) can also be used to detect the presence of N.
Gonorrhoeae in all specimen types except urine.If Gram-negative, oxidase-positive diplococci are visualized on direct Gram stain of urethral pus (male genital infection), no further testing is needed to establish the diagnosis of gonorrhea infection. However, in the case of female infection direct Gram stain of cervical swabs is not useful because the N. Gonorrhoeae organisms are less concentrated in these samples. The chances of false positives are increased as Gram-negative diplococci native to the normal vaginal flora cannot be distinguished from N. Thus, cervical swabs must be cultured under the conditions described above. If oxidase positive, Gram-negative diplococci are isolated from a culture of a cervical/vaginal swab specimen, then the diagnosis is made. Culture is especially useful for diagnosis of infections of the throat, recutum, eyes, blood, or joints – areas where PCR-based tests are not well established in all labs.
Culture is also useful for antimicrobial sensitivity testing, treatment failure, and epidemiological purposes (outbreaks, surveillance).In patients who may have disseminated gonococcal infection (DGI), all possible mucosal sites should be cultured (e.g., pharynx, cervix, urethra, rectum). Three sets of blood cultures should also be obtained. Synovial fluid should be collected in cases of.All people testing positive for gonorrhea should be tested for other sexually transmitted diseases such as,. Studies have found co-infection with ranging from 46 to 54% in young people with gonorrhea. For this reason, gonorrhea and chlamydia testing are often combined. People diagnosed with gonorrhea infection have a fivefold increase risk of HIV transmission. Additionally, infected persons who are HIV positive are more likely to shed and transmit HIV to uninfected partners during an episode of gonorrhea.
ScreeningThe (USPSTF) recommends screening for gonorrhea in women at increased risk of infection, which includes all sexually active women younger than 25 years. Extragenital gonorrhea and chlamydia are highest in (MSM). Additionally, the USPSTF also recommends routine screening in people who have previously tested positive for gonorrhea or have multiple sexual partners and individuals who use condoms inconsistently, provide sexual favors for money, or have sex while under the influence of alcohol or drugs.Screening for gonorrhea in women who are (or intend to become) pregnant, and who are found to be at high risk for, is recommended as part of. See also:As with most sexually transmitted diseases, the risk of infection can be reduced significantly by the correct use of and can be removed almost entirely by limiting sexual activities to a mutually monogamous relationship with an uninfected person.Those previously infected are encouraged to return for follow up care to make sure that the infection has been eliminated.
In addition to the use of phone contact, the use of email and text messaging have been found to improve the re-testing for infection.Newborn babies coming through the birth canal are given ointment in the eyes to prevent blindness from infection. The underlying gonorrhea should be treated; if this is done then usually a good prognosis will follow. Treatment Antibiotics. Entered mass production in 1944 and revolutionized the treatment of several venereal diseases.Antibiotics are used to treat gonorrhea infections. As of 2016, both by injection and by mouth are most effective.
However, due to increasing rates of, local susceptibility patterns must be taken into account when deciding on treatment.Adults may have eyes infected with gonorrhoea and require proper personal hygiene and medications. Addition of topical antibiotics have not been shown to improve cure rates compared to oral antibiotics alone in treatment of eye infected gonorrhea. For newborns, ointment is recommended as a preventative measure for gonococcal infant. Among persons in the United States between 14 and 39 years of age, 46% of people with gonorrheal infection also have chlamydial infection.Infections of the throat can be especially problematic, as antibiotics have difficulty becoming sufficiently concentrated there to destroy the bacteria. This is amplified by the fact that pharyngeal gonorrhoea is mostly asymptomatic, and gonococci and commensal Neisseria species can coexist for long time periods in the pharynx and share anti-microbial resistance genes.
Accordingly, an enhanced focus on early detection (i.e., screening of high-risk populations, such as men who have sex with men, should be considered) and appropriate treatment of pharyngeal gonorrhoea is important. Sexual partnersIt is recommended that sexual partners be tested and potentially treated. One option for treating sexual partners of people infected is (PDPT), which involves providing prescriptions or medications to the person to take to his/her partner without the health care provider's first examining him/her.The United States' currently recommend that individuals who have been diagnosed and treated for gonorrhea avoid sexual contact with others until at least one week past the final day of treatment in order to prevent the spread of the bacterium.
Antibiotic resistance. Main article:Many antibiotics that were once effective including, and are no longer recommended because of high rates of resistance. Resistance to has reached a level such that it is no longer recommended as a first-line agent in the United States, and if it is used a person should be tested again after a week to determine whether the infection still persists. Cases of resistance to ceftriaxone have been reported but are still rare, though public health officials are concerned that an emerging pattern of resistance may predict a global epidemic. The UK's reported that 2011 saw a slight drop in gonorrhea antibiotic resistance, the first in five years.
143Gonorrhea if left untreated may last for weeks or months with higher risks of complications. One of the complications of gonorrhea is systemic dissemination resulting in skin or,. This occurs in between 0.6 and 3% of infected women and 0.4 and 0.7% of infected men.In men, and can result from untreated gonorrhea. In women, the most common result of untreated gonorrhea is. Other complications include, a rare complication associated with; in the fingers, wrists, toes, and ankles;; during pregnancy; neonatal or adult blindness from;.
Men who have had a gonorrhea infection have an increased risk of getting. Gonorrhea—Rates: United States, 1941–2007About 88 million cases of gonorrhea occur each year, out of the 448 million new cases of curable STI each year – that also includes syphilis, chlamydia.
In 2013, it caused about 3,200 deaths, up from 2,300 in 1990.In the United Kingdom, 196 per 100,000 males 20 to 24 years old and 133 per 100,000 females 16 to 19 years old were diagnosed in 2005. In 2013, the CDC estimated that more than 820,000 people in the United States get a new gonorrheal infection each year. Fewer than half of these infections are reported to CDC.
In 2011, 321,849 cases of gonorrhea were reported to the CDC. After the implementation of a national gonorrhea control program in the mid-1970s, the national gonorrhea rate declined from 1975 to 1997. After a small increase in 1998, the gonorrhea rate has decreased slightly since 1999. In 2004, the rate of reported gonorrheal infections was 113. 5 per 100,000 persons.In the US, it is the second-most-common bacterial; remains first.
According to the CDC are most affected by gonorrhea, accounting for 69% of all gonorrhea cases in 2010.The World Health Organization warned in 2017 of the spread of untreatable strains of gonorrhea, following analysis of at least three cases in Japan, France and Spain, which survived all antibiotic treatment. During World War II, the U.S. Government used posters to warn military personnel about the dangers of gonorrhea and other.Some scholars translate the biblical terms zav (for a male) and zavah (for a female) as gonorrhea.It has been suggested that was used as a treatment for gonorrhea.
Surgeons' tools on board the recovered English warship the included a that, according to some, was used to inject the mercury via the into any unfortunate crewman suffering from gonorrhea. The name 'the clap', in reference to the disease, is recorded as early as the sixteenth century, referring to a medieval in Paris, Les Clapiers. Translating to 'The rabbit holes', it was so named for the small huts in which prostitutes worked.In 1854, Dr. Addressed gonorrhea in his book, Homeopathic Guide to all Diseases Urinary and Sexual Organs. He noted that the disease was common in and in large cities. Gollmann recommended the following as cures: to cure 'shooting pains with soreness and inflammation;' mercury 'for stitching pain with purulent discharge;' and 'when the symptoms are complicated with and stricture of the. Other include, aurum , and.was one of the widely used drugs in the 19th century.
However, it became replaced. Invented this type of colloidal silver, which was marketed by from 1897 onward. The silver-based treatment was used until the first antibiotics came into use in the 1940s.The exact time of onset of gonorrhea as prevalent disease or epidemic cannot be accurately determined from the historical record. One of the first reliable notations occurs in the Acts of the (English) Parliament. In 1161, this body passed a law to reduce the spread of '.the perilous infirmity of burning'. The symptoms described are consistent with, but not diagnostic of, gonorrhea.
A similar decree was passed by in France in 1256, replacing regulation with banishment. Similar symptoms were noted at the by.Coincidental to, or dependent on, the appearance of a gonorrhea epidemic, several changes occurred in European medieval society. Cities hired doctors to treat afflicted patients without right of refusal. Rescinded the requirement that physicians complete studies for the lower orders of the.Medieval public health physicians in the employ of their cities were required to treat prostitutes infected with the 'burning', as well as lepers and other epidemic victims. After Pope Boniface completely secularized the practice of medicine, physicians were more willing to treat a sexually transmitted disease. ResearchA vaccine for gonorrhea has been developed that is effective in mice. It will not be available for human use until further studies have demonstrated that it is both safe and effective in the human population.
Development of a vaccine has been complicated by the ongoing evolution of resistant strains and antigenic variation (the ability of N. Gonorrhoeae to disguise itself with different surface markers to evade the immune system).As is closely related to and they have 80–90% homology in their genetic sequences some cross-protection by is plausible. A study published in 2017 showed that group B meningococcal vaccine provided a partial protection against gonorrhea. The vaccine efficiency was calculated to be 31%.

